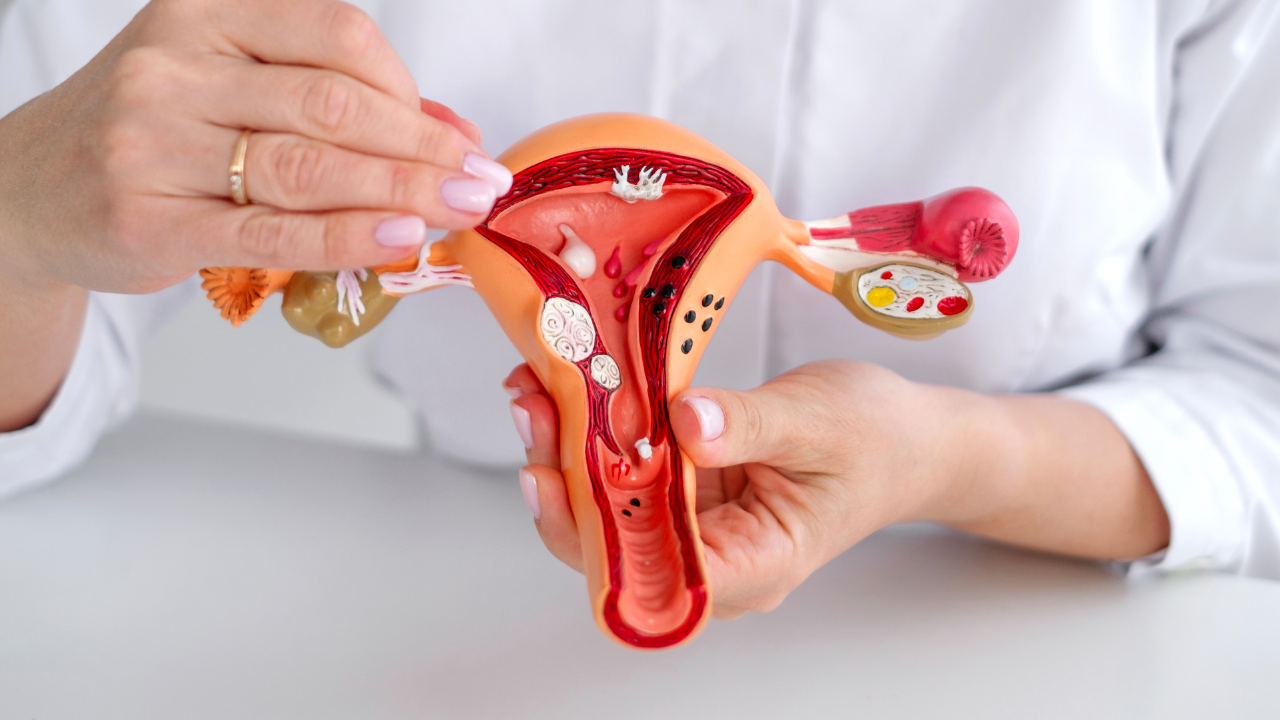
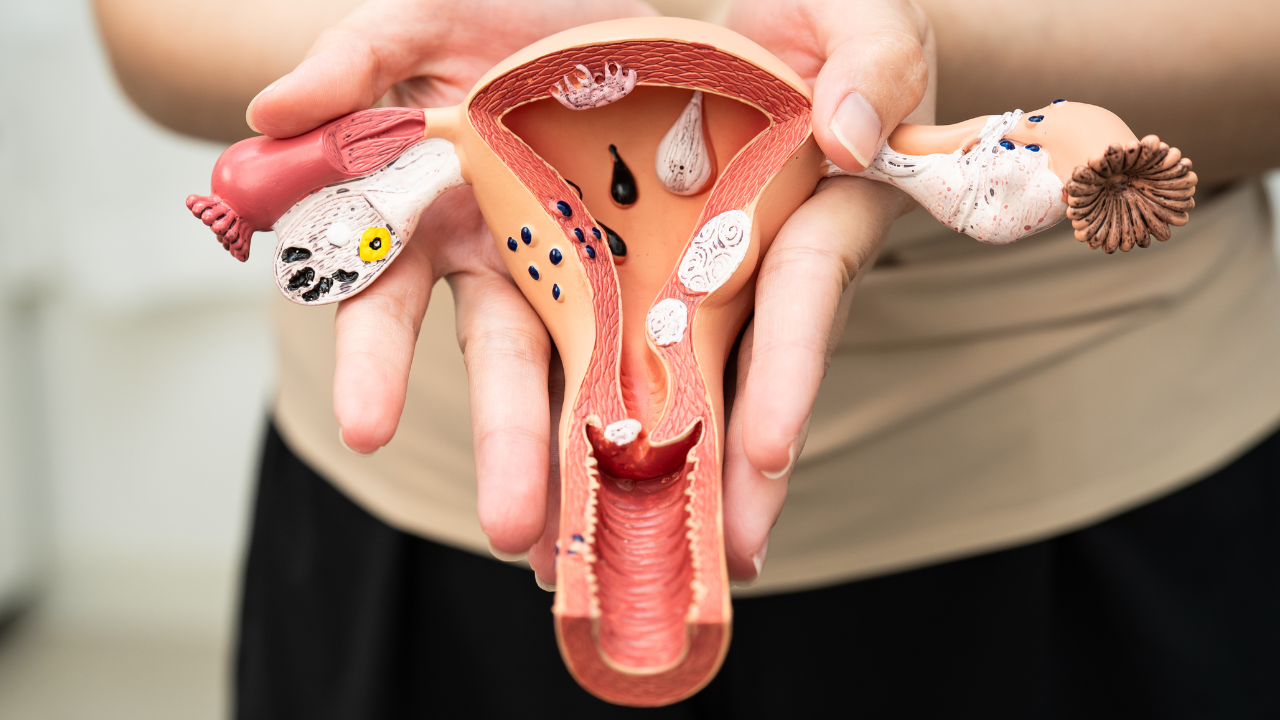
By Dr Hamon Ng, fertility specialist at City Fertility Melbourne
Adenomyosis is a common yet often misunderstood condition that affects many women and individuals assigned female at birth. It can cause a range of symptoms and may have important implications for fertility. Accurate diagnosis and a clear understanding of available treatment options are key to managing the condition effectively. In this blog, Dr Hamon Ng shares expert insights into adenomyosis, including its symptoms, impact on fertility and quality of life and treatment options
What is Adenomyosis?
Adenomyosis is an oestrogen-responsive condition that affects up to 1 in 5 people assigned female at birth, making it more common than endometriosis. It is commonly found in women over 30 years old, with the risk of adenomyosis increasing after pregnancy or following uterine surgery.
Adenomyosis occurs when endometrial tissue that lines the uterus grows into the muscular wall of the uterus. This tissue continues to act as it normally would, thickening, breaking down and bleeding during each menstrual cycle. This can cause the uterine muscle to thicken and enlarge, sometimes doubling in size, and may lead to heavy menstrual bleeding and pain.
Understanding the underlying mechanisms of adenomyosis is essential for accurate diagnosis and effective management of this condition. Whilst there is no cure for adenomyosis, we can manage its symptoms and improve the quality of life for those diagnosed.
What Causes Adenomyosis?
The exact cause of adenomyosis remains unclear. We know that it only affects those who menstruate and is usually diagnosed in people over 30 years. Uterine disruption associated with prior surgical procedures, such as pregnancy termination or caesarean delivery, is considered a potential mechanism in the pathogenesis of adenomyosis.
Other proposed causes of adenomyosis include invasion of endometrial tissue into the muscular wall of the uterus, uterine injury or disruption, inflammatory and immune-mediated processes, hormonal influences (particularly oestrogen), and developmental factors arising early in life. The development of adenomyosis is likely multifactorial, with a combination of these mechanisms contributing to disease onset and progression.
What are the Symptoms of Adenomyosis?
Adenomyosis typically appears from the age of 35 into the 40’s, and the symptoms vary widely in intensity. While some individuals may experience no symptoms at all, others may face debilitating challenges. Common symptoms include:
- An enlarged uterus, which can create a lower belly bulge (often referred to as an adenomyosis belly)
- Heavy or prolonged menstrual bleeding
- Severe cramping or sharp, knife-like pelvic pain during menstruation (dysmenorrhea)
- Longer than normal menstrual cycles
- Pain during sex (dyspareunia)
- Abdominal tenderness
- Chronic pelvic pain, often a central, heavy, cramping pelvic pain that varies in intensity
- Referred leg pain
- Anaemia or iron deficiency (due to heavy periods), leaving you feeling tired or dizzy.
- Difficulty trying to conceive
What are the Differences Between Adenomyosis and Endometriosis?
There’s often confusion between adenomyosis and endometriosis because they share many similarities. Despite this, they are very different conditions.
Both conditions involve tissue similar to the lining of the uterus and are driven by oestrogen, which is why they have similar symptoms, such as heavy periods, pelvic pain, painful periods, and fertility challenges. Because of this, it’s not always easy to tell them apart based on symptoms alone.
They’re also frequently found together, so some people may have both conditions at the same time, which can further blur the distinction.
The key difference is location: endometriosis occurs outside the uterus, whereas adenomyosis occurs within the uterine muscle. Understanding the difference helps guide accurate diagnosis and treatment planning.
| Adenomyosis | Endometriosis | |
|---|---|---|
| Location | Inside the uterine wall or myometrium. | Outside the uterus. |
| Symptoms | |
|
| Diagnosis | First line ultrasound. Can consider MRI. | Ultrasound or laparscopy. |
| Effect on fertility | May adversely affect fertility especially through impairing embryo implantation | Known association/correlation with infertility |
| Treatment | Complementary therapy (Yoga, physio, accupuncture etc.)Non hormonal medications (simple analgesia), hormonal medications (Mirena IUD, COCP, POP etc.) IVF can be considered for fertility | Complementary therapy (Yoga, physio, accupuncture etc.)Non hormonal medications (simple analgesia), hormonal medications (Mirena IUD, COCP, POP etc.), Surgical excision (Laparoscopy). IVF for fertility |
How Does Adenomyosis Affect Fertility?
Adenomyosis is not always a direct cause of infertility, but it can be associated with fertility challenges for some people. The condition may create inflammation and or changed conditions within the uterus, which can hinder implantation of a fertilised egg, and hormonal changes that may impact ovulation or egg quality.
It’s important to know that many people with adenomyosis are still able to conceive, and a diagnosis does not mean you won’t be successful. Likewise, there is no reason not to proceed with IVF if you have adenomyosis, and many patients are still successful.
For those who are not ready to start a family yet, egg freezing (Oocyte cryopreservation ) may be an option to help preserve your fertility for the future. Oocyte cryopreservation may facilitate fertility preservation at a younger reproductive age, enabling patients to proceed with essential adenomyosis treatment without compromising future reproductive options.
If you have adenomyosis and want to have a baby now or are concerned about the future, an appointment with a fertility specialist can help you understand your individual situation and explore the most appropriate options for your reproductive goals.
What are the Treatments for Adenomyosis?
Treatment strategies for adenomyosis aim to alleviate symptoms and improve overall well-being. Treatment also depends on an individual’s reproductive goals and age.
Adenomyosis affects 20% of individuals assigned female at birth, and for some, it can have a profound effect on daily life. Greater awareness of the symptoms and treatment options for adenomyosis empowers individuals to seek timely care and support, improving the quality of life for those affected.
Management of adenomyosis in individuals wishing to preserve or achieve fertility requires a carefully individualised approach that balances symptom control with reproductive goals. Conservative measures aimed at improving quality of life may include simple analgesia, such as paracetamol and non-steroidal anti-inflammatory medications, to help manage dysmenorrhoea and pelvic pain. Complementary strategies, including pelvic physiotherapy, regular exercise, optimisation of sleep, psychological support, mindfulness-based therapies, and dietary measures with an anti-inflammatory focus, may also provide symptomatic benefit for some individuals. Where symptoms are significant, short-term hormonal suppression may occasionally be considered in carefully selected cases, although treatment choice must take into account the potential impact on ovulation and timing of conception attempts.
For those experiencing infertility or when conception is delayed, assisted reproductive treatment may play an important role in management. Ovulation induction or intrauterine insemination may be appropriate in selected circumstances; however, in moderate to severe adenomyosis, in older reproductive age groups, or where additional fertility factors are present, in vitro fertilisation (IVF) is often the most effective treatment option. IVF may help overcome some barriers to conception by facilitating embryo creation and transfer under closely monitored conditions, although adenomyosis can still affect implantation and miscarriage risk through its effects on the uterine environment. In some cases, pretreatment strategies aimed at reducing adenomyosis activity prior to embryo transfer may improve reproductive outcomes, and fertility preservation options such as oocyte or embryo cryopreservation may also be considered where treatment delay or disease progression is a concern.
There is currently limited high-quality evidence evaluating the benefit of specific dietary interventions for adenomyosis. However, some studies suggest that a diet rich in anti-inflammatory and antioxidant-containing foods may support overall reproductive and pelvic health. This includes foods high in omega-3 fatty acids, such as oily fish, nuts, and seeds, as well as colourful vegetables, whole grains, and foods containing adequate vitamin D. While dietary modification should not be considered a primary treatment, it may serve as a supportive strategy as part of a broader, individualised management approach.
For individuals with adenomyosis who are not currently seeking pregnancy, treatment is primarily focused on symptom control, improving quality of life, and limiting disease progression where possible. Initial management often includes simple analgesia, such as paracetamol and non-steroidal anti-inflammatory medications, to reduce menstrual pain and pelvic discomfort. Complementary measures—including regular exercise, pelvic physiotherapy, stress reduction, optimisation of sleep, and dietary strategies with an anti-inflammatory focus—may provide additional symptomatic benefit. Hormonal treatments are frequently central to management and may include the oral contraceptive pill, progestogen therapies, the levonorgestrel intrauterine device (Mirena), or GnRH-based therapies (Zoladex, etc.), which aim to suppress hormonal stimulation of adenomyosis tissue and reduce heavy menstrual bleeding, pain, and uterine inflammation.
Where future fertility is desired but not immediate, treatment planning should also consider long-term reproductive goals. In some individuals, fertility preservation strategies such as oocyte or embryo cryopreservation may be considered prior to prolonged hormonal suppression, advancing maternal age, or interventions that may impact reproductive potential.
Frequently Asked Questions about Adenomyosis
Adenomyosis can be definitively cured with hysterectomy (surgical removal of the uterus), as this removes the source of the condition. However, for many individuals, symptoms can be effectively managed without hysterectomy through a range of treatments including simple analgesia, hormonal therapies, complementary measures, and, in very selected cases, conservative surgical management. Treatment is individualised based on symptom severity, age, fertility goals, and disease extent, with the aim of improving quality of life and controlling symptoms.
Whilst adenomyosis isn’t life-threatening, for some people it can be life-impacting, especially if symptoms like heavy bleeding and severe pain are significant. The good news is that there is support and effective treatments available, particularly if diagnosed early.
Getting pregnant naturally with adenomyosis can be challenging, but it is possible. Adenomyosis is associated with hormonal imbalances, particularly excess estrogen, an irregular menstrual cycle, affecting ovulation and embryo implantation issues. A fertility specialist can assess your hormones and ovulation. They can help balance your hormones with diet and lifestyle modifications, and if required, progesterone support to improve natural conception.
Adenomyosis has not been directly linked as a cause of infertility. Despite this, some individuals with adenomyosis do struggle to conceive. The two most common fertility concerns relate to ovulation disorders, and displaced endometrial tissue can create an inflammatory environment within the uterus, potentially hindering the implantation of a fertilised egg.
Yes, it is possible to have both adenomyosis and endometriosis, with estimates that up to 40-80% of women with endometriosis also have adenomyosis. Historically, adenomyosis has tended to be a disorder diagnosed in a slightly older population, although more recently, younger patients are presenting with a diagnosis of adenomyosis on ultrasound. It is also quite common for patients initially to present with endometriosis, particularly those with the more severe form of the disease, who then, years later, develop adenomyosis.