By Dr Andrew Zuschmann, specialist at City Fertility Miranda
If you’ve been diagnosed with endometriosis, or you’re worried you might have it it’s completely normal to have questions about what this means for your fertility. Many people assume that endometriosis automatically means infertility, but that’s not always the case.
Let’s break it down in a way that’s easy to understand.
So, what exactly is endometriosis?
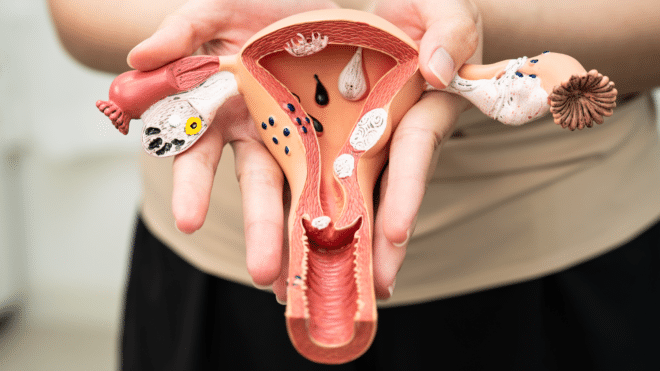
Endometriosis is a long-term condition where tissue similar to the lining of the uterus grows outside the uterus. These areas are most often found on the ovaries, fallopian tubes, or elsewhere in the pelvis, in particular on the peritoneum, which is the “glad wrap” that lines our abdominal cavity.
Because this tissue responds to hormones, it can swell and become inflamed during the menstrual cycle. Over time, this can lead to pain, inflammation, and scarring.
Endometriosis is actually very common, affecting around 1 in 9 people assigned female at birth, but it’s often underdiagnosed. Many people spend years being told their pain is “normal” before getting answers.
Does endometriosis affect fertility?
It can, but not always.
Endometriosis can affect fertility in a few different ways. It may change the anatomy of the pelvis, block the fallopian tubes, affect ovulation or egg quality, or create inflammation that makes it harder for fertilisation or implantation to occur.
Mechanical blockages
Endometriosis can lead to scar tissue (adhesions) forming within the pelvis. These adhesions may block the fallopian tubes, preventing the egg and sperm from meeting—or distort the ovary, which can interfere with normal egg release.
Inflammation
Endometriosis is associated with ongoing inflammation in the pelvis. This can result in the release of inflammatory chemicals (such as cytokines) that may negatively affect egg and sperm quality, fertilisation, and early embryo development.
Ovarian involvement (endometriomas)
When endometriosis affects the ovaries, cysts known as endometriomas can form. These may reduce ovarian reserve (the number of eggs available) and can also impact egg quality.
Implantation difficulties
Endometriosis can alter the environment of the uterus. Changes to the uterine lining may make it more difficult for an embryo to implant successfully.
Hormonal and immune changes
The condition can disrupt normal hormonal balance and immune function, both of which play important roles in conception and early pregnancy.
That said, the severity of endometriosis doesn’t reliably predict fertility. Some people with significant endometriosis conceive naturally, while others with mild disease may need support.
Age, overall health, and lifestyle factors also play a big role.
What treatments are available if you’re trying to get pregnant?
There’s no single “right” treatment for endometriosis. Management needs to be tailored to your symptoms, your goals, and where you are in life.
Many people with endometriosis will become pregnant without any specific treatment, but if you’re experiencing delays it’s important to have make an individualised plan discussing the options of surgery or IVF, and the pros and cons of each specific to you.
Surgery is undertaken with a keyhole approach, aiming to restore anatomy, and remove deposits of endometriosis
It’s usually fine to continue pain relieving medication for endometriosis if you’re trying to get pregnant, but we avoid hormonal treatments as they’ll typically prevent pregnancy.
Multidisciplinary care including pelvic physiotherapy, dietary changes, or acupuncture may also be recommended.
Can you minimise the impact of endometriosis on fertility with lifestyle?
While lifestyle changes can’t “cure” endometriosis, they can help minimise its impact on fertility by supporting overall reproductive health and reducing inflammation. Maintaining a healthy weight, exercising regularly, getting good-quality sleep, and managing stress can all play a role.
Some people find that dietary changes such as reducing ultra-processed foods, limiting alcohol, and focusing on whole foods (including vegetables, fibre, and omega-3 fats) may improve symptoms and wellbeing.
If pain is affecting daily life or intimacy, pelvic physiotherapy can also be helpful with pelvic muscle dysfunction that can develop in response to chronic pain. Working alongside a gynaecologist or fertility specialist, physiotherapy can help we can help improve pelvic mobility
Acupuncture may support some people with endometriosis by helping to reduce pelvic pain and inflammation, improve blood flow to the reproductive organs, and regulate the nervous system. These effects may enhance overall wellbeing and help create a more supportive environment for fertility, even though evidence for a direct improvement in pregnancy rates remains limited.
The key is a personalised approach that supports your fertility goals alongside medical care. You can read more practical strategies in our guide on how to increase your fertility.
For more information on endometriosis and common causes of female infertility, visit our page here. If you have concerns about endometriosis and fertility we recommend an appointment with a City Fertility specialist. To discuss your situation with a specialist or call 1300 354 354
When might IVF be recommended?
For some people, IVF is the most effective way to achieve a pregnancy.
IVF may be recommended if endometriosis is affecting fertility, or if there are other factors involved such as tubal damage, ovulation issues, male factor infertility, or unexplained infertility.
IVF involves fertilising an egg with sperm in a laboratory, then transferring a healthy embryo back into the uterus. While it can sound daunting, many people find reassurance in having a clear plan forward.
The takeaway
Endometriosis doesn’t automatically mean you won’t be able to have children. Many people conceive naturally, and others do so with fertility treatment.
What really matters is early assessment, good information, and an individualised approach.
If you’re living with endometriosis and thinking about your fertility, whether now or in the future, you don’t have to navigate it alone. Booking a consultation with a City Fertility specialist to understand your options and create a plan tailored to you.







