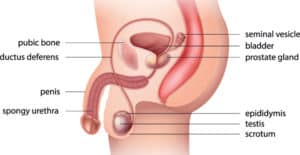
Understanding the male reproductive system
For a couple to conceive a baby, both the male and female reproductive systems must be functioning properly. In the male this means:
- The testes produce viable, or normal, sperm as well as testosterone, the male hormone.
- The ability to achieve an erection and engage in sexual intercourse.
- Normal ejaculation occurs, with semen going through the man’s urethra into the vagina.
- The sperm that are produced are properly shaped, able to move rapidly, and can accurately go to the fallopian tubes to find and fertilise the egg.
Testes
The testes are two glandular organs responsible for making testosterone – the primary male sex hormone – and for generating sperm. Most men have two testes, which are suspended in the scrotum by the spermatic cords. Within the testes are coiled masses of material called seminiferous tubules. These tubes are responsible for producing sperm cells.
Epididymis
The epididymis is a single, narrow, tightly coiled tube (six to seven metres long) connecting the efferent ducts from the rear of each testicle to its vas deferens. It transports and stores sperm cells produced in the testes. The epididymis also brings the sperm to maturity, since the sperm that emerge from the testes are immature and incapable of fertilisation.
Vas deferens
The vas deferens connects the left and right epididymis to the ejaculatory ducts to move sperm. Each tube is about 30cm long and muscular, and travels from the epididymis into the pelvic cavity, to just behind the bladder. During ejaculation the smooth muscle in the wall of the vas deferens contracts, pushing the mature sperm towards the penis and into the urethra.
Urethra
The urethra is the tube that carries urine from the bladder to outside the body, and is about 20cm long. When the penis is erect during sex, the flow of urine is blocked from the urethra, allowing only semen to be ejaculated at orgasm.
Accessory glands
The male accessory glands are: seminal vesicles, prostate gland and bulbourethral glands.
- Seminal vesicles: These are found within the pelvis and their function is to secrete a significant proportion of the fluid that ultimately becomes semen.
- Prostate gland: The prostate secretes a slightly alkaline fluid, milky or white in appearance, which normally constitutes 50% to 75% of the volume of the semen.
- Bulbourethral glands: The function of these glands is to produce a clear, salty, viscous secretion (pre-ejaculate) during sexual arousal, to help to lubricate the urethra for spermatozoa to pass through. This fluid neutralises traces of acidic urine in the urethra and helps to remove any residual urine or foreign matter.
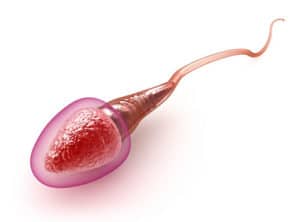
Sperm is the male reproductive cell that binds and fertilises a woman’s egg to produce an embryo. It consists of a head, midpiece and tail. The head contains chromosomes that will bind with the egg’s chromosomes to determine an offspring’s characteristics. Sperm also carry the X or the Y chromosome that will determine the gender of the resulting child. The tail gives the sperm cell movement and helps it to travel to, and then penetrate, the egg.
Sperm cells may survive in the female reproductive tract for two to three days.
Semen is the fluid produced by the male reproductive tract that dilutes the concentrated sperm at ejaculation. Semen also contains other factors produced by various male glands that bathe and nourish the sperm to keep it viable.
A Semen analysis evaluates the amount and quality of a man’s semen and sperm to determine his fertility. The test looks at the volume, count, motility, morphology and pH of semen and the sperm it contains.
This can give an indication of how successful your sperm may be at fertilising an egg, and what method of fertility treatment your specialist may recommend.
The World Health Organisation has set a reference guide for the standardisation of semen analysis globally. A semen sample is considered “normal” when: it exceeds 1.5ml in volume; more than 15 million sperm are counted per millilitre of semen; more than 50% of the sperm are moving in a progressively forward motion; and more than 4% of the sperm have a normal morphology (shape). *WHO 2010.
To learn more about male screening tests, visit our Sperm test & semen analysis page.
Request an appointment with one of our specialists.Make your appointment