By Professor William Ledger, an internationally renowned fertility specialist at City Fertility Sydney CBD.
Contrary to what we would expect, some women with the most severe endometriosis have been found to conceive naturally and have a good pregnancy, while some with milder cases of the condition struggle to conceive. So while there is often a link established between endometriosis and fertility, it is not always the case.
However, when fertility issues are evident, and a woman has been diagnosed with endometriosis, undergoing surgery for the endometriosis can often improve the chances of natural fertility.
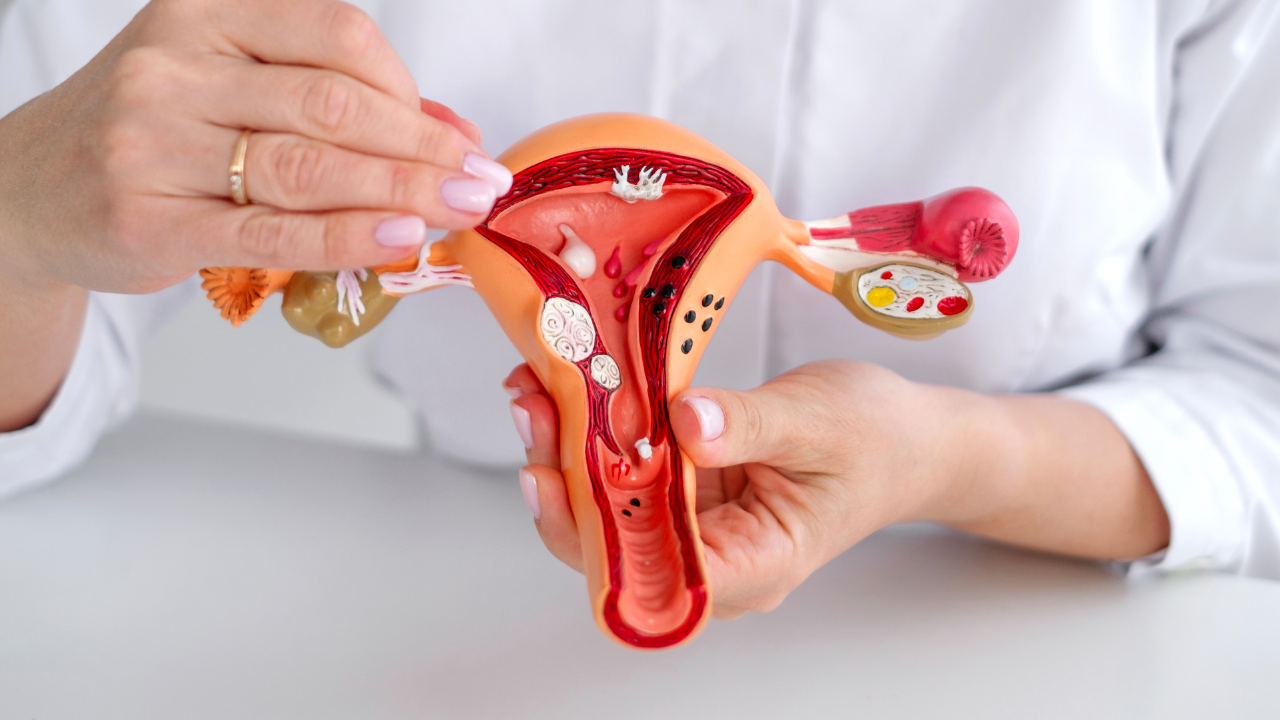
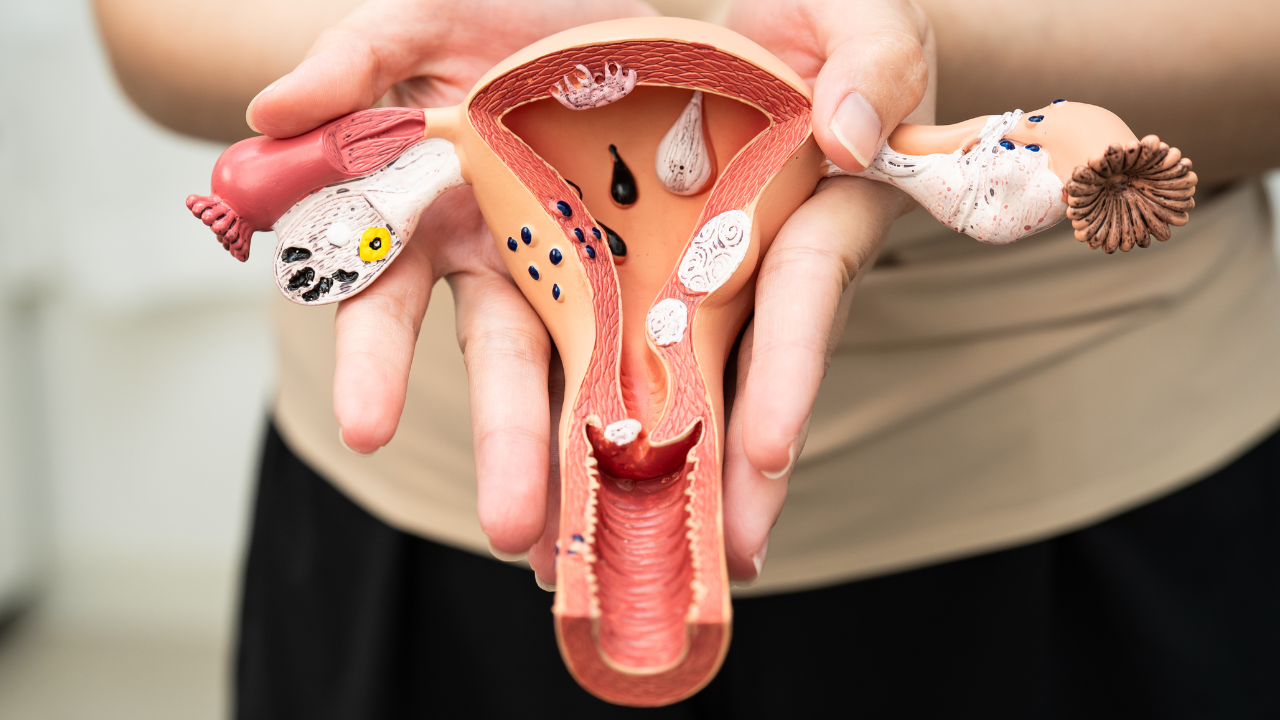
Endometriosis varies considerably in its severity and in its impact on a woman’s health. Endometriosis occurs when tissue similar to the tissue that normally lines inside of the uterus — the endometrium — grows outside the uterus, and the condition is graded from mild (level 1) to severe (level 4).
Why can endometriosis sometimes impact fertility?
It is not fully clear why some women with the milder form of the disease struggle to conceive naturally, but a problem often exists and surgical correction may help. The impact of moderate and severe endometriosis on fertility probably results from distortion of the normal anatomy.
For example, a large endometriotic cyst on an ovary can interfere with the process of ovulation and pickup of the oocyte (egg) by the Fallopian tube.
Is surgery the solution?
There has only ever been one well designed trial of laparoscopic (keyhole) surgery to treat mild endometriosis in women with fertility problems – the ‘Endocan’ study from the 1990s – and this showed a benefit of surgical correction. It is thought mild endometriosis may have a toxic effect on oocytes (eggs) and following surgery (and minimisation of the endometriosis) this might account for this benefit and improvement in chances.
Endometriosis often also causes pain, including pain with intercourse, which can obviously interfere with trying to conceive. Again, surgery can often improve this problem.
Are there increased risks when trying to fall pregnant?
Not really, apart from the impact of fertility problems. Endometriosis usually becomes quiet during pregnancy due to hormones from the placenta. Many women with endometriosis find that their pain subsides and they feel much better. Bladder and bowel function may improve. However, sadly, this is not a ‘cure’ and problems usually recur once the baby is delivered. Breast feeding can inhibit ovulation and prevent resumption of periods, so if period related pain is a feature, it’s a good idea to plan to breast feed for several months if possible.
Can anything be done to minimise the impact of endometriosis on fertility?
A sad story that we frequently hear is of severe monthly period pain in a teenage schoolgirl, which is not taken seriously in primary care. Later, the more grown up woman seeks help and is diagnosed with endometriosis which has been present for many years and has had considerable impact on her health and wellbeing.
It is easy to organise an abdominal ultrasound to investigate unexplained abdominal pain in young women, and to suppress progression of endometriosis problems using contraceptive pills or other medications. This can have significant benefit later when she wishes to conceive.
For adults with endometriosis, it may be worthwhile freezing eggs before major surgery or considering medical management with progestogens or a GnRH agonist. This however needs careful discussion with a specialist.
Can endometriosis symptoms vary?
The range of symptoms and problems we can see in different patients with endometriosis is phenomenal.
One woman with grade 4 disease can be pain-free and leading a normal life, but is diagnosed when investigated for fertility problems. Another patient will have mild disease but will need major painkillers and several surgeries to help improve her health.
As we don’t yet have a blood test that can diagnose the disease so we still rely on scanning (ultrasound and MRI) and laparoscopy to work out if there is a problem and, if so, how severe.
For more information on endometriosis and common causes of female infertility visit here or to discuss your situation with one of our specialists or call 1300 354 354