The 25th July is recognised as World Embryologist Day, the same special date as the world’s first IVF baby being born.
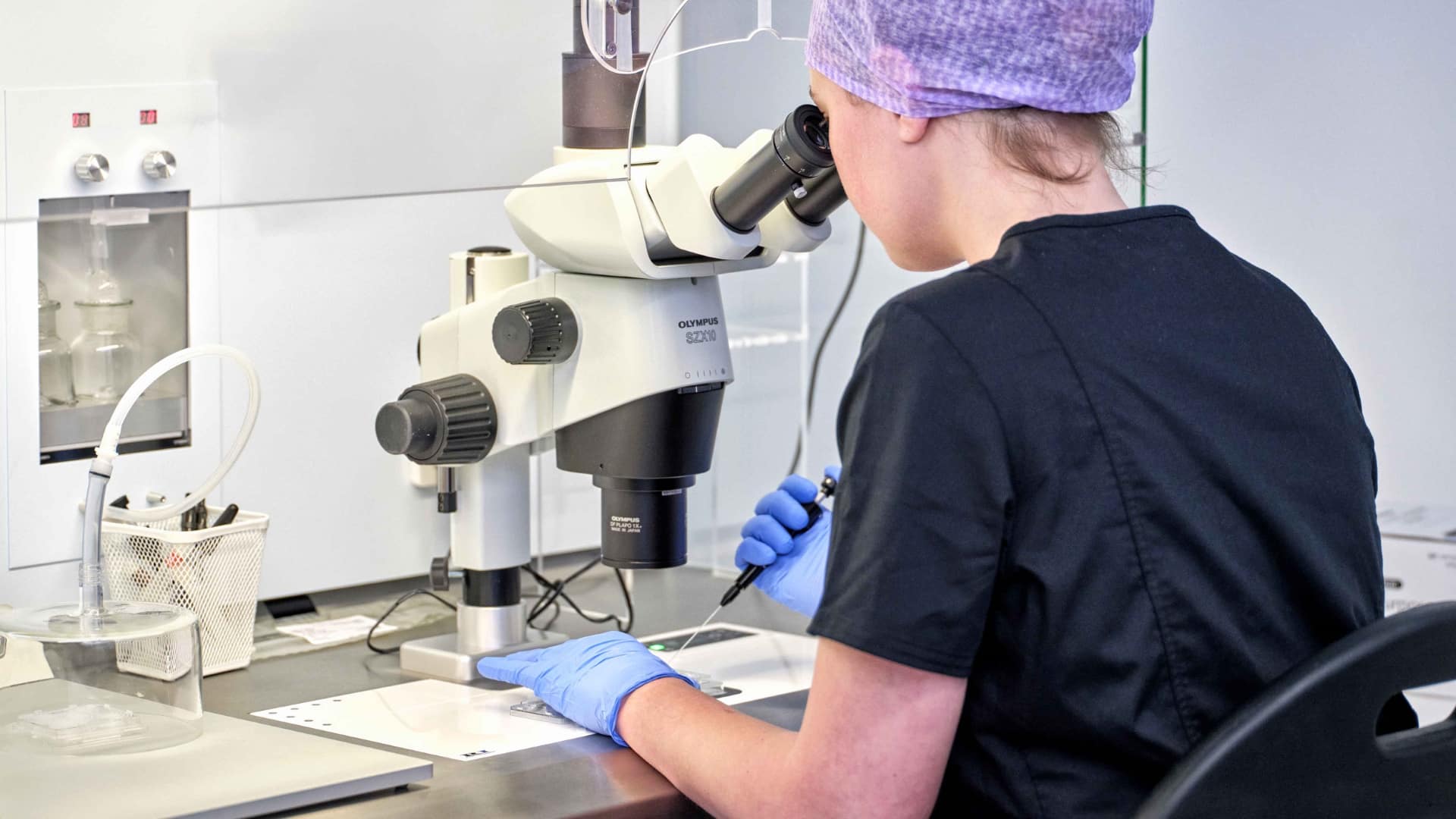
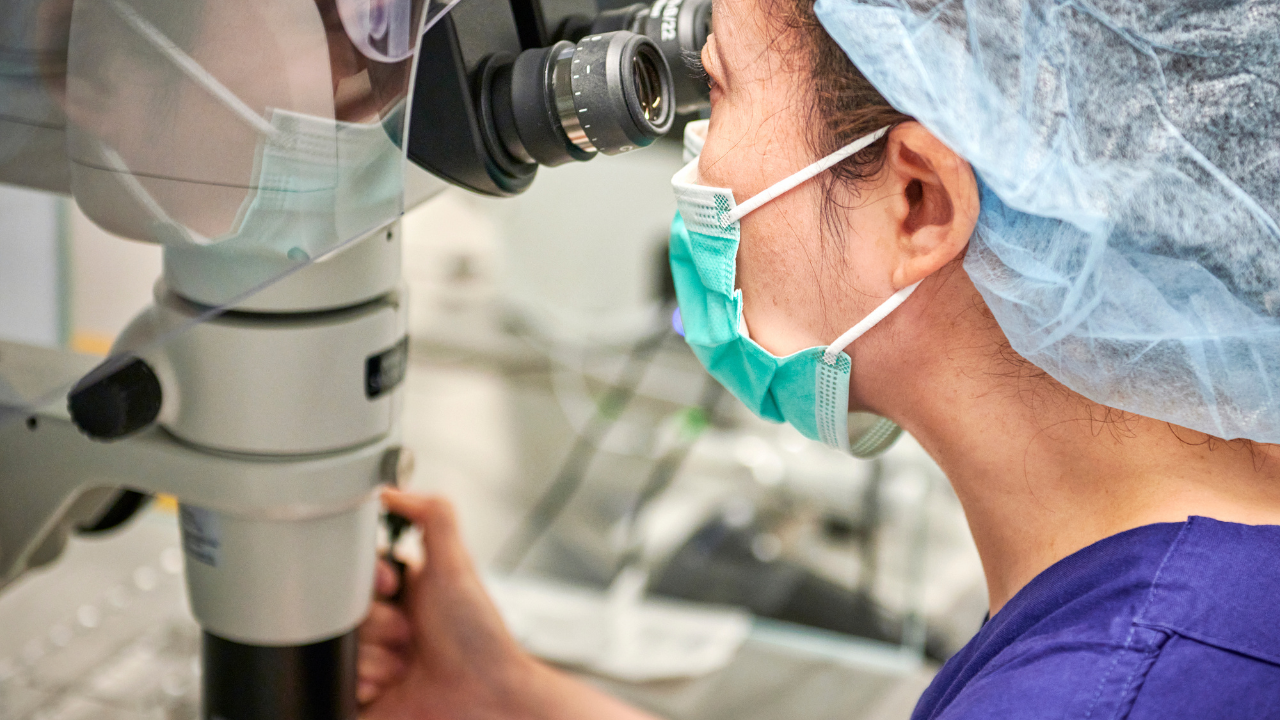
Embryologists play a critical role in an IVF clinic – they are the scientific staff who help make babies happen, literally creating life in their hands. They are sometimes referred to as the ‘caretakers’ of a patient’s sperm, eggs or embryos because they are the nurturers of this new start of life.
However, embryologists don’t only work in the laboratory, they are also in regular direct communication with our patients too, whether that be at the first information session, at egg retrieval, to update patients of how their embryos are progressing, then again face-to-face at embryo transfer. Embryologists are the link in the chain whose hands create your baby for you.
Cheryl Ayres, Senior Embryologist at City Fertility, said it is a real privilege to be involved in the whole IVF process.
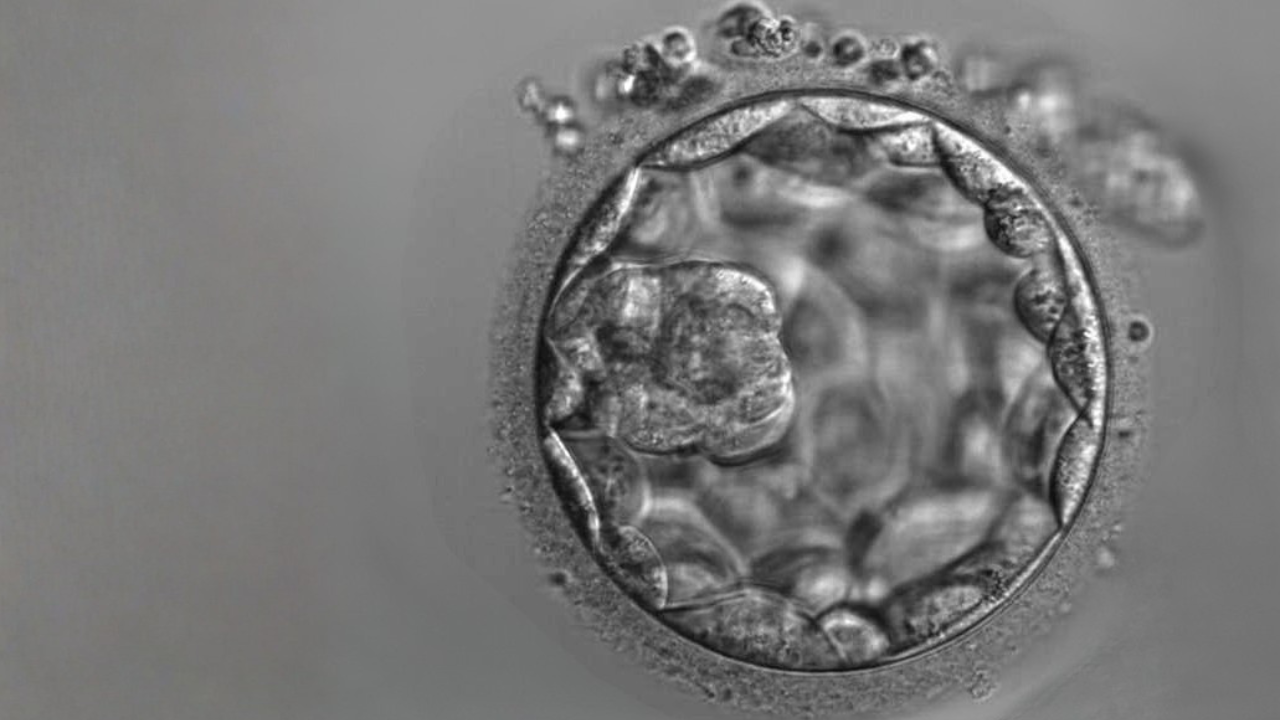
“It’s really wonderful to be a part of a patients’ fertility journey, whether that is as a role in supporting the couple, or in the lab creating and then caring for the embryos from start to finish. It’s magnificent when we see the embryo at five days old before transfer, and then the next time we meet, it is a little baby and that’s an amazing feeling and why I love my job so much,” said Ms Ayres.
Here are some of the task embryologists carry out as part of their important role in an IVF clinic:
One part of an embryologist’s role is to undertake semen analysis testing, which evaluates the quality of a man’s ejaculate and the sperm cells within it. This test is sometimes called a sperm count. Under a microscope, the embryologists will assess: Motility: movement of the sperm (swimming ability); Morphology: reported as a percentage of sperm that have a normal shape; and the Count: the number of individual sperm present in one ejaculation. The combined result of all this information is part of the process in being able to move forward with types of treatment options for the patients.
On the day of egg collection or insemination, the embryologists will also prepare the semen sample provided by the partner on the day to isolate the best quality sperm for insemination.
Before an egg collection, a patient will meet one of the embryologists’ face-to-face, to discuss what the treatment plan created for them by the clinician entails. During an egg collection (or egg retrieval, or egg pick up) fluid is aspirated from the follicles on the ovary by the clinician. This fluid which may contain the eggs, is then passed to the embryologist for examination under a microscope in order to identify and collect the eggs. The embryologist will then keep the clinician notified of a running total of eggs found during the procedure.
The embryologists are responsible for putting the eggs and sperm together on the same day as egg collection, to attempt fertilisation and start embryo formation. This can be done in a couple of different ways, mainly depending on the sperm quality. In conventional IVF a calculated number of prepared sperm are put into the dish containing the patient’s eggs and the sperm then swim to the egg and attempt to fertilise it. Alternatively, if using ICSI as the mechanism of insemination, the embryologist undertaking the procedure is responsible for selecting the sperm that will be microinjected into the egg thus bypassing any issues associated with sperm count or motility, or for all of the issues relating to sperm and oocyte interaction.
The day after the sperm and eggs are carefully placed together, the embryologist then checks these eggs for evidence of fertilisation (this means the egg and sperm have genetically combined to create the start of an embryo) by examining each of them under the microscope. They will then call the patient as soon as they can to give them their fertilisation result.
The embryologists then replace these fertilised eggs back into ideal culture conditions inside an incubator, which is regulated to control temperature and maintain a pH that mimics the condition of the uterus. These optimal conditions enable the fertilised egg to continue to grow and to develop into an embryo. The embryos are then checked every other day, and the embryologists will also refresh the culture media as required to help maintain optimal embryo growth and development.
If required, the embryologist may help with assisted hatching during the culture phase. This is recommended in a few cases, the outer shell of the embryo known as zona pellucida is thinned with the help of a laser in order create a “weak” point in the shell to facilitate the embryo hatching out and allowing implantation to occur.
Transfer usually occurs on day 5, when the embryologists will assess all of the patient’s embryos in culture, and will select the best quality embryo(s) and when the transfer is taking place, will load them into the transfer catheter. This loaded catheter is then carefully handed over to the fertility specialist who will select the location to place the embryo(s) safely inside the uterine cavity. Usually this is completed under ultrasound guidance with embryo release happening in the optimum location within the uterus by the embryologist.
Embryos created within a treatment cycle that are excess to requirements and are of suitable quality, or indeed eggs and sperm themselves, can be frozen to preserve them for later use. The embryologists suspend the embryo (usually at the blastocyst stage), or egg, in a tiny drop of fluid on a specialised tool which allows for rapid freezing. The droplet is lowered onto a metal block that has been cooled by liquid nitrogen, where it then hardens into a glass-like bead. This prevents ice crystal formation which could fracture or shatter delicate embryo cells. Sperm is frozen either in straws or in amps, using a different specialised media which also acts to protect and prevent them from undergoing cryoshock, but are frozen using a different process.
When requested. embryologists can carry out pre-implantation genetic diagnosis (PGD) of embryos before they are implanted to assess for any chromosomal abnormalities in the embryos. The most common embryo testing method happens on day 5 or 6 of embryo development and is called embryo biopsy, where some blastomeres, or embryonic cells, are carefully removed from the growing embryo and then tested for their genetic profile. All embryos undergoing PGD are frozen to allow time for the genetic report to be profiled and completed. If testing reveals a normal genetic profile, then this embryo would be one chosen to be transferred. Any other normal profile embryos will remain frozen for future use if required. Also, in some instances, just the eggs can be genetically tested before fertilisation occurs, however this is much less common.
Ensuring the laboratories run and maintain optimum conditions is imperative to minimise disruption to eggs, sperm and embryos and to maximise pregnancy outcomes. Our embryologists carefully maintain the temperature inside the incubators and of equipment used to monitor these embryos, along with the humidity and gas levels within these incubators too, as well as the overall lab air quality with a range of technologies. They also maintain our time-lapse incubators to optimise embryo development and hence also patient outcomes and results.
Another role, as part of maintaining the laboratory environment, is for the embryology team to look after the frozen embryos, eggs and sperm in our cryostorage tanks to ensure that they are maintained in a different kind of controlled environment, to ensure that they remain viable. These tanks are monitored regularly by our teams to ensure that liquid nitrogen levels remain optimum to ensure that frozen stock stays frozen. These tanks are also kept locked with only embryologists having access to them, and then, of course, these are kept securely either in the laboratory itself or within a specialised room designed especially for their ongoing storage.
Request an appointment with one of our specialists.Make your appointment