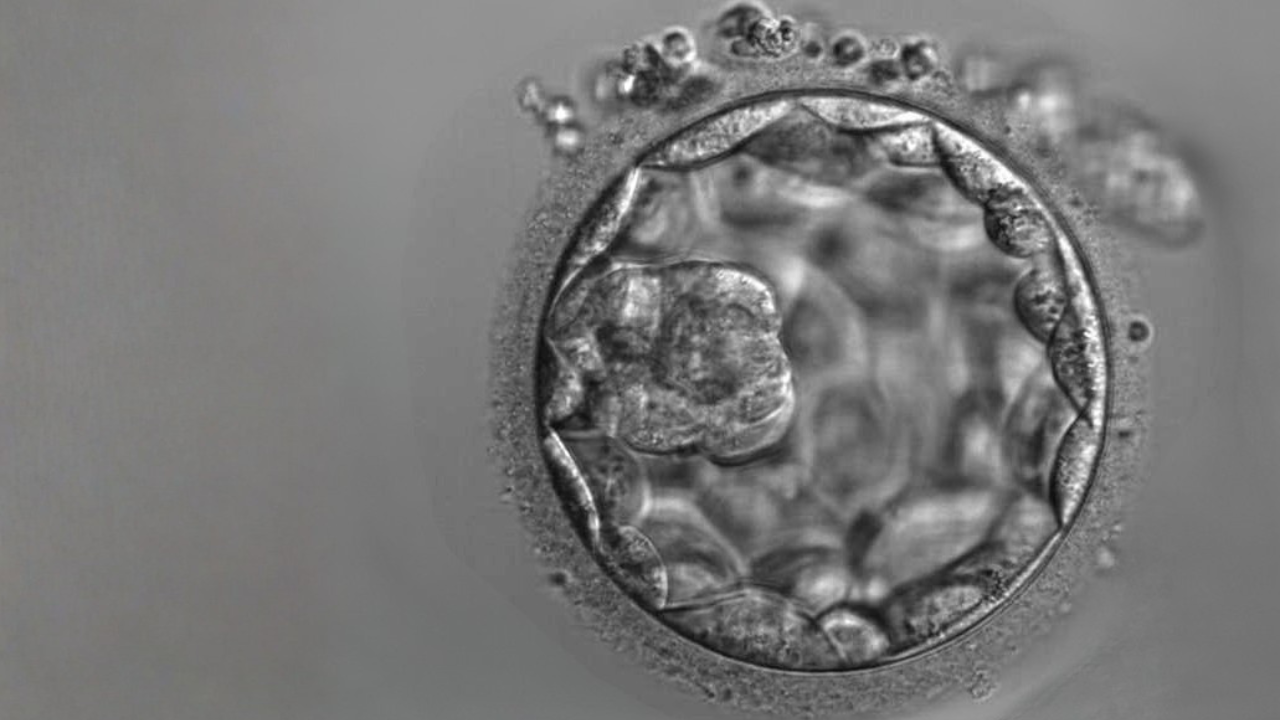
IVF has been around for 40 years and is now commonly used worldwide to help bring healthy babies into the world.
Medical interventions and technologies are used frequently in all types of medical procedures today, and IVF is just one of these that can help towards a happy outcome.
IVF literally means “fertilisation in glass”, except today it is no longer in glass, it is in plastic. The process involves fertilising the egg with the sperm in an incubator outside the body, then transferring the best embryo back into the woman’s uterus. The whole process, up to the embryo transfer stage, usually takes three to four weeks.
If after an initial consultation (testing and diagnosis) your specialist determines that IVF is the best plan for you, then below are the normal steps that the treatment will follow.
During a regular menstrual cycle, hormones from the pituitary gland – Luteinising Hormone (LH) and Follicle Stimulating Hormone (FSH) – cooperate in the growth and release of an egg from a fluid-filled follicle within the ovary. While numerous follicles start growing each month, only one will become mature enough to ovulate. Ovulation (release of the egg from the ovary) is caused by an increase in LH about two weeks before menstruation starts.
On the other hand, during an IVF cycle, it is desirable for several eggs to mature at the same time with FSH injections, with a trigger injection given to mature the developing eggs before collection. Hence the need for “pituitary suppression”.
There are different forms of IVF treatment: with pituitary suppression before starting stimulation (sometimes called long downregulation), and with pituitary suppression after the stimulation has started (sometimes called the antagonist cycle).
Your treating specialist will have selected the best cycle type for your individual needs.
Your fertility coordinator will provide you with detailed information about your specific treatment cycle, including the timeline and medications. You will also be shown how to administer your daily FSH injections and given instructions for any other medications you may need during your treatment cycle.
This stage involves stimulating the ovaries with medication to promote the growth of follicles containing eggs. This is done via daily FSH injections for between 9 and 14 days. The FSH dose used is slightly higher than what a woman naturally produces – this is to stimulate the growth of multiple follicles.
The response of the ovaries is monitored with regular ultrasounds and blood tests. Most women learn to administer their own injections, or their partner may assist, which helps reduce the number of clinic visits.
The ovarian stimulation phase ends once ultrasounds show that the number and size of the follicles are adequate. The FSH injections and the GnRH agonist/antagonist (pituitary suppressant) are then stopped. Once your fertility coordinator has confirmed your procedure time with the theatre, he or she will advise the exact time to administer your trigger injection. This is an injection of human chorionic gonadotropin (hCG) to aid the egg’s final maturation and loosen it from the follicle wall.
Egg retrieval takes place on the second morning after the final injection (34-36 hours later). Your trigger injection timing is crucial, so ensure you record it carefully along with your instructions.
Your specialist will then perform the egg retrieval or egg “pick-up” while you are lightly sedated. This involves passing an ultrasound-guided probe, with a fine needle attached, through the vaginal canal and into each follicle in the ovary. The fluid in the follicle is then extracted into a test tube and studied under a microscope to look for eggs.
This procedure takes 20 to 30 minutes, depending on the number of developed follicles. After the egg retrieval, you will rest for one hour before going home. City Fertility Centre recommends patients take the day off work and avoid any strenuous exercise.
On the day of your egg retrieval procedure, your partner will be asked to produce his semen sample. A men’s room is available at each City Fertility Centre clinic. If you and your partner have any concerns about collecting the sample, please discuss this with staff before starting your cycle. It may be possible to produce the sample at home and drop it off at the clinic, or freeze one of your partner’s semen samples as a backup.
Next, the sperm sample is washed and concentrated, then added to the eggs about four hours after egg retrieval. The sperm and eggs are placed in an incubator overnight, and the eggs are examined the next day for signs of fertilisation. Usually, 60 to 70 per cent of eggs will fertilise if the sperm sample appears normal.
An embryologist will contact you to discuss fertilisation outcomes and any questions you may have. The fertilised eggs are then kept in the incubator for an additional 48 hours.
Your treating specialist may suggest Intracytoplasmic Sperm Injection (ICSI) as part of your treatment if the sperm quality is low (sperm count, morphology or motility). ICSI is a specialised form of treatment for male infertility and involves injecting a single sperm directly into a single mature egg.
Embryo transfer occurs two to five days after egg retrieval. The embryo chosen for transfer is inserted into a thin plastic catheter (a soft tube), which is passed through the cervix and into the uterus, then gently released. The process itself takes only a few minutes and is usually painless.
Generally, only one embryo is transferred, or two in exceptional cases – this will depend on your individual circumstances and embryo quality.
After the transfer, some of the remaining embryos may be suitable for vitrification (rapid freezing), and this option is available to all patients undergoing IVF treatment. Frozen embryos can be used in subsequent cycles if the first cycle is unsuccessful. To be suitable for freezing, embryos must not show signs of abnormal/slow development or fragmentation (cell breakdown).
The luteal phase is the two-week period between the embryo transfer and the pregnancy test. During this time, it is important that you look after yourself and maintain good health and wellbeing. You will be encouraged to limit strenuous activity for 24 hours after the transfer.
The progesterone medication you start taking after egg retrieval can sometimes cause tiredness, nausea, cramping and bloating. You may choose to take an analgesic if you experience any discomfort. If you are concerned about any symptoms, contact your fertility centre and speak with a fertility coordinator.
Vaginal spotting or bleeding may happen before you are due for your pregnancy test, but this does not always mean treatment was unsuccessful. You should continue using any treatment medications until a full period begins and/or you and your specialist have received your blood test results.
Your pregnancy blood test is due about 14 days after the embryo transfer. Your nurse will phone to give you the results and advise you on the next steps in your journey to having a child.
We recognise that the time between embryo transfer and your pregnancy test can be emotionally charged with anxiety and expectation. We understand this can be a difficult time, and encourage you to call your clinic for support if you are finding it hard to cope with the stress of waiting. Access to professional counsellors is also available as part of your IVF treatment.
We provide personalised, compassionate care and will support you at every step of your fertility journey.
For more information on the cost of treatment, potential risks, who IVF is recommended for, and to download a step-by-step infographic of the process, please visit our IVF treatment page.