If you are already going through the process of IVF with the help of a fertility specialist and embryologist, when and why should you consider taking the next step to have your embryos diagnosed for potential issues? Below, we outline, in simple terms, your options, how they are done, and the potential risks.
Pre-implantation Genetic Screening (PGS) can be very beneficial for a range of patients, including those with:
- Recurrent miscarriage
- Advanced maternal age
- A family history of chromosomal disorders
- Previous unsuccessful IVF cycles
- A desire to increase their chance of a successful cycle
- Severe male infertility
- A family history of X-linked disease.
If embryos have abnormal chromosomes, this may prevent implantation to the uterine lining (endometrium) or lead to early pregnancy loss, or (less likely) result in the birth of a child with disabilities.
PGS detects anomalies in the number or structure of chromosomes in embryos. This allows the selection of the best embryos for implantation, also known as Advanced Embryo Selection (AES). Generally, we are dealing with an extra whole chromosome (trisomy), or a whole chromosome missing (monosomy).
The potential benefits of AES and choosing only chromosomally normal embryos include:
- Lessening the risk of a live-born child with a chromosomal abnormality
- Lowering the incidence of miscarriage
- Improving IVF success rates by prioritising chromosomally “normal’’ embryos for transfer
- Reducing the number of IVF cycles required to achieve a successful outcome
- Supporting elective single-embryo transfer to reduce multiple pregnancies.
More specific Pre-implantation Genetic Diagnosis (PGD) is available for the majority of serious (single-gene) genetic conditions and is recommended if patients want to test for a known genetic disease of which they are, or potentially are, a carrier.
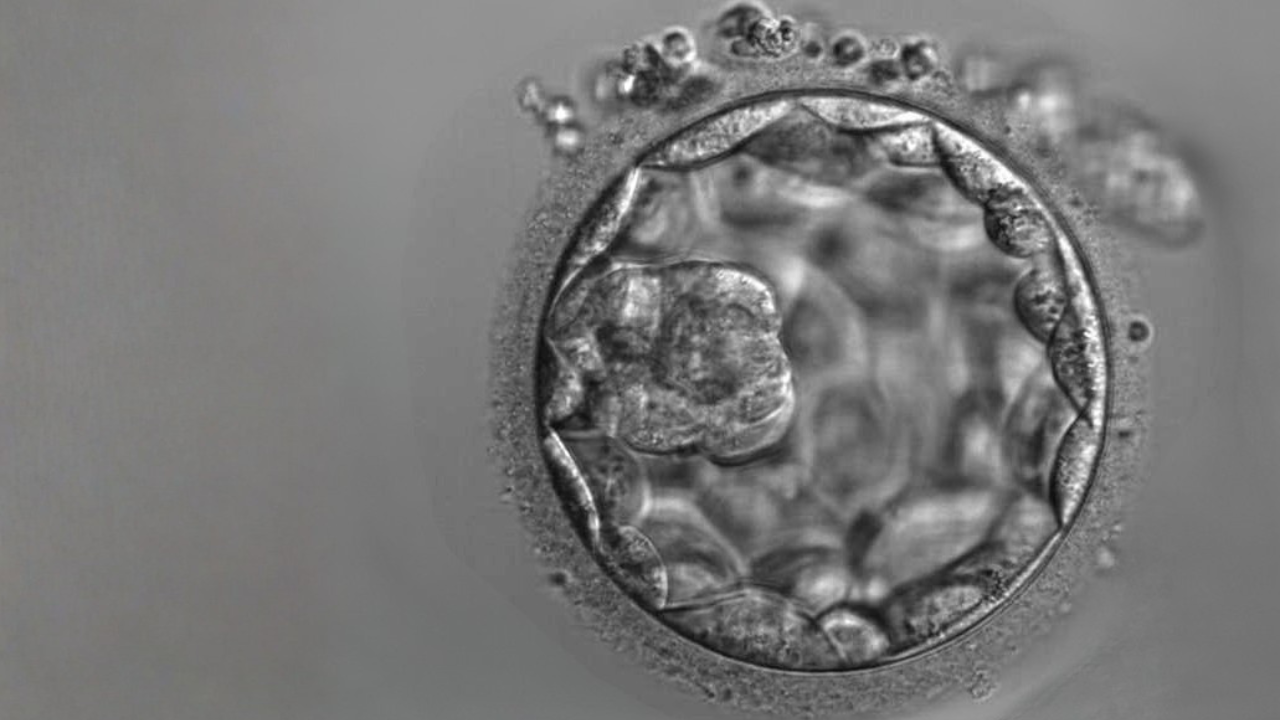
The most common embryo testing method is blastocyst biopsy, whereby a few cells are carefully removed from the trophectoderm (destined to be the membranes and placenta) on the fifth to seventh day of embryo development, and then tested in our laboratory.
Another available method is polar body biopsy, where the maturing egg produces two small cells known as polar bodies, which degenerate after fertilisation. The polar bodies are carefully removed and the chromosomal content tested. This is rarely performed and is used to check egg quality.
The biopsied cells are analysed via PGS techniques called Comparative Genomic Hybridisation (CGH) or Fluorescence In-Situ Hybridisation (FISH).
The CGH testing method looks at all chromosomes, including the X and Y, and compares them with a sample of “normal” DNA. A computerised scanner interprets the test results, which are then verified by a scientist. CGH can test all 23 pairs of chromosomes.
The FISH method uses probes labelled with different fluorescent dyes. The number of chromosomes is counted and the geneticist can distinguish the normal cells and those with aneuploidy (an extra or missing chromosome). FISH is able to test only a limited number of chromosomes.
While the testing of the cells is taking place, the embryos are frozen and kept in storage.
If the testing reveals normal embryos, then the best-quality one is chosen to be thawed and transferred. The remaining viable embryos with normal results will remain frozen for future use.
Embryos with abnormal results are discarded. Sometimes the testing process reveals a mosaic embryo, and other times the technology fails to give a result at all. In these two latter situations, careful discussion with your doctor is essential.
The associated risks of blastocyst biopsy are low. The risk of accidental damage to an embryo during removal of cells in the hands of an experienced embryologist is very low, and is currently less than 1%.
No part of the future fetus will be affected because only a few cells are removed, and cells are taken only from the trophectoderm.
The accuracy of PGS for aneuploidy is about 98%, which means there is an error rate of 2%. Due to this small chance of misdiagnosis, we recommend prenatal testing as well.