By Dr Peng Ng, fertility specialist at City Fertility Brisbane Southside
Modern medicine is a wonderful thing, whether it is creating lives or saving lives, it never ceases to amaze. These medical advances are ever-present in fertility medicine and one of the interesting facts about seeking fertility help in this era is that there are now so many different methods and treatments that can increase your chances of achieving a pregnancy.
One of these fertility treatments is Intracytoplasmic Sperm Injection, or ICSI, as many people call it, and it is a type of IVF that has been helping create babies for the past 30 years. So why is ICSI different to straight IVF and what does it involve? Here is a quick guide to help enlighten you.
A specialised form of IVF
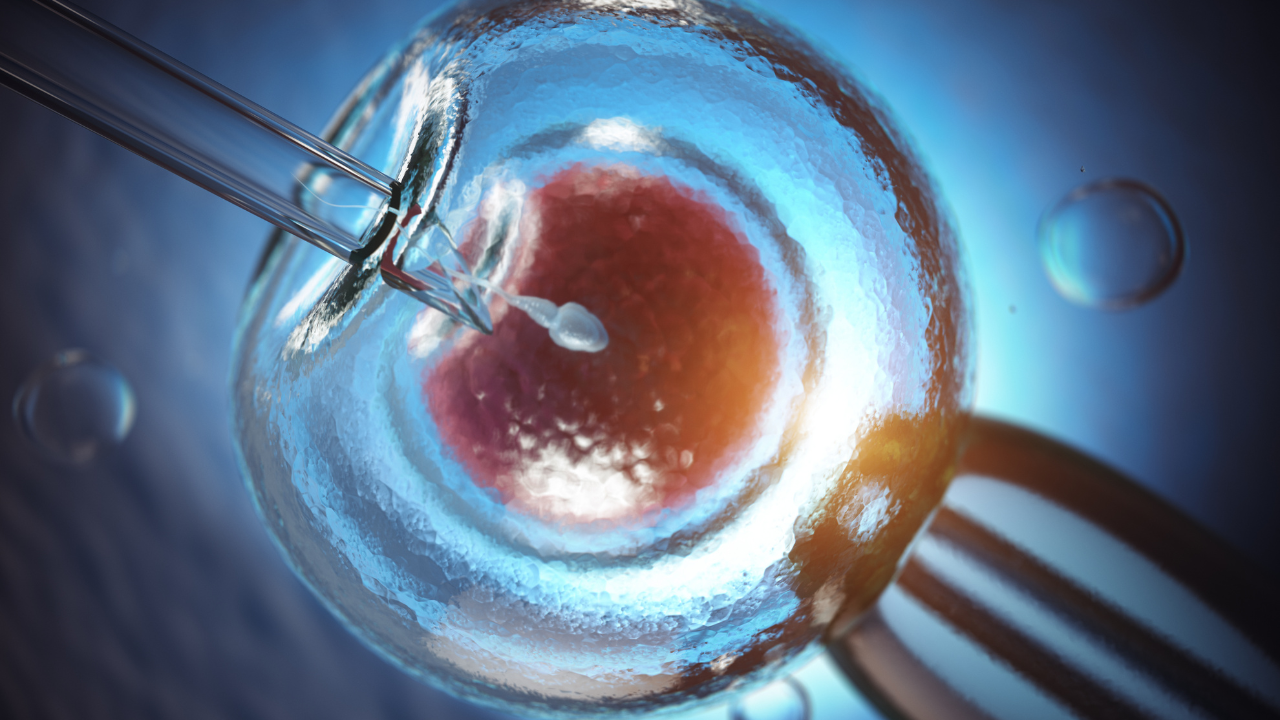
ICSI is a specialised form of In Vitro Fertilisation (IVF) that is used primarily for the treatment of severe cases of male-factor infertility. It involves the injection of a single sperm directly into a mature egg. In contrast, IVF relies on the egg and the sperm being left in a petri dish to fertilise on their own accord.
At City Fertility, we use a medium named Sperm Slow™ during sperm selection. This medium contains hyaluronan (HA), which binds sperm that are more likely to have normal DNA, and thus allows selection of these bound sperm for injection. By selecting sperm bound to HA and using them for ICSI, the embryologists preferentially use the better-quality, more mature sperm. Please note that, while this technique using HA is standard practice, it may not be suitable in every case, depending on individual circumstances.
About 30 per cent of all infertility is due to a significant male-factor problem. ICSI has revolutionised the treatment of male infertility. Before the first successful ICSI pregnancy in 1992, little could be offered to couples with severe male-factor infertility, aside from using donor sperm.
Who is ICSI recommended for?
ICSI is recommended for couples who have had poor or no fertilisation during standard IVF.
In addition, it is recommended for men who have any of the following known concerns: poor sperm morphology (abnormally shaped sperm); Poor sperm motility (slow-moving); a low sperm count; An obstruction such as a vasectomy, which prevents sperm release; anti-sperm antibodies (which are produced by the man’s body and may inhibit sperm function); a vasectomy reversal that was unsuccessful or resulted in a low sperm count or poor-quality sperm.
What are the steps?
Step 1: The female ovaries are stimulated with medication to help promote the growth of follicles containing eggs.
Step 2: The mature eggs are retrieved from the female partner during a standard IVF cycle.
Step 3: The male partner’s sperm is selected – a semen sample is prepared in the laboratory to isolate as many healthy, moving sperm as possible.
Step 4: After the eggs have rested for two to three hours, following their removal from the female, the tight outer coating (cumulus) is gently removed from each egg so the maturity of the eggs can be clearly observed. The genetically mature eggs are selected.
Step 5: The embryologist then injects a single sperm previously selected into the mature egg.
Step 6: The injected eggs (in dishes) are placed in the incubator overnight and checked for fertilisation 16-18 hours later.
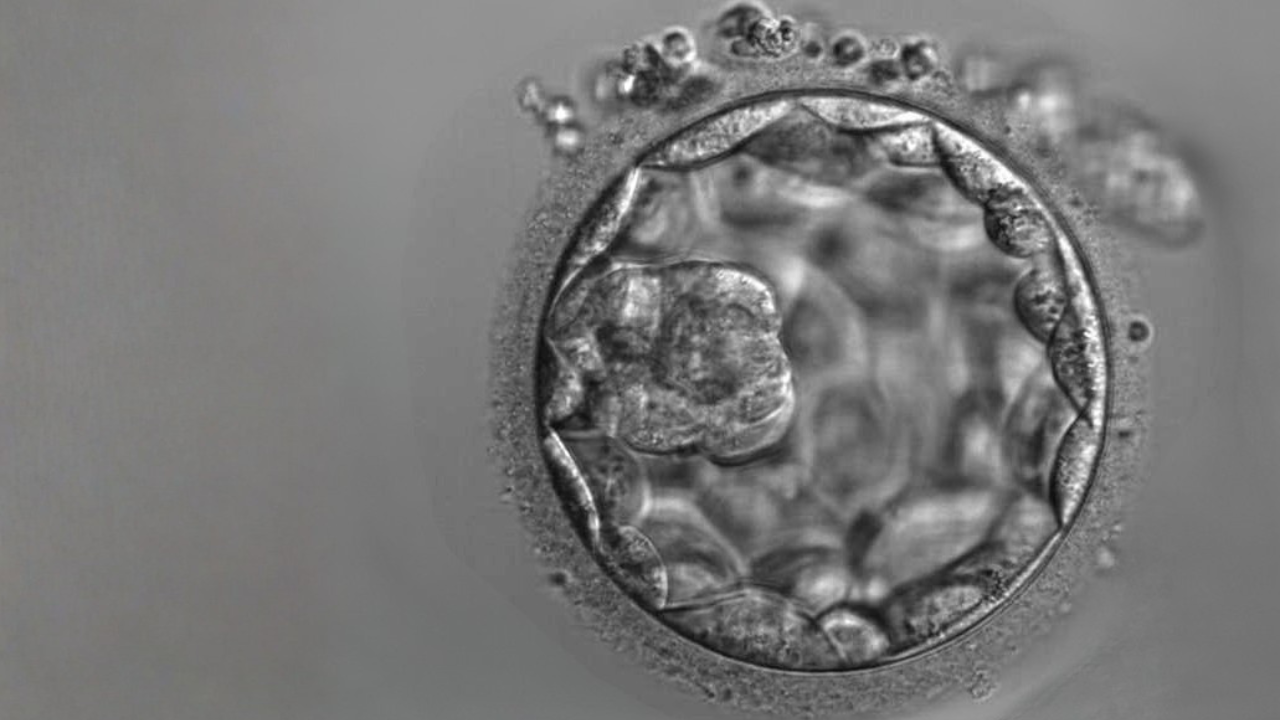
Step 7: Those that have fertilised are then left in the incubator to continue to grow for 2-5 days.
Step 8: An embryo is then chosen for transfer. It is loaded into a transfer catheter and placed into the uterus. Generally, only one embryo is transferred and in exceptional cases two.
Step 9: Any remaining good-quality embryos can be vitrified (frozen) and stored for subsequent cycles if the first cycle is not successful.
Step 10: A pregnancy test is then carried out approximately 14 days after the embryo transfer.