City Fertility supports the Jean Hailes Women’s Health Week (6-10 September) which is dedicated to all women across Australia to make good health a priority.
If you’re currently focusing on your fertility health or planning ahead, then there are plenty of things you can do to enhance your fertility and a range of treatments available if and when you need it.
The desire to become a parent is independent of sex, sexuality or gender identity, and there are also many different paths to parenthood, whether as a couple, shared or sole parenting, and they also include adoption, foster care and surrogacy.
According to Dr Devora Lieberman, fertility specialist and Medical Director of City Fertility NSW clinics, “planning and starting a family is a deeply personal, emotional and exciting time but it’s no secret that trying for a baby can bring some unexpected challenges to your journey towards parenthood.”
“We need to better understand how challenging it can be to get pregnant. From our teens to early 20s we tend to take precautions to avoid pregnancy and then tend to overestimate our fertility when we decide we’re actually ready to conceive.”
“Age is a key factor in a woman’s chance to conceive so the older you are when you’re ready to start a family, the harder it can become.”
“Even at the young age of 22, a woman will have about a 25 per cent chance of conceiving each month, and by about 35, that’s down to about 15 to 20 per cent. By 42, half of us won’t be able to get pregnant at all with our own eggs.”
According to Dr Lieberman, “The best test that we have for fertility is to try to get pregnant. Sometimes it’s simply about getting heterosexual couples to have sex at the right time.
“If you’re trying to get pregnant, have sex every other day in the typical 28-day cycle from day 8 to day 16. Sperm will live in the fallopian tubes for at least three days and be capable of fertilising an egg. An egg only has about a 12 to 24-hour window in which it can fertilise. You want the sperm to be waiting for the egg.
We encourage you to learn about the causes, symptoms and treatments available, then you can better understand your situation and have more control of the journey,” Dr Lieberman says.
Common signs and symptoms of infertility include:
- Trying to become pregnant for six to twelve months
- Irregular or absent menstrual periods
- History of pelvic infection
- Two or more miscarriages
- History of using an IUD for birth control
- Sterilisation reversal
- Difficulties with sexual intercourse
- Chronic pelvic pain
- Breast discharge
- History of sexually transmitted disease
- Excessive acne or facial hair
- PCOS diagnosis
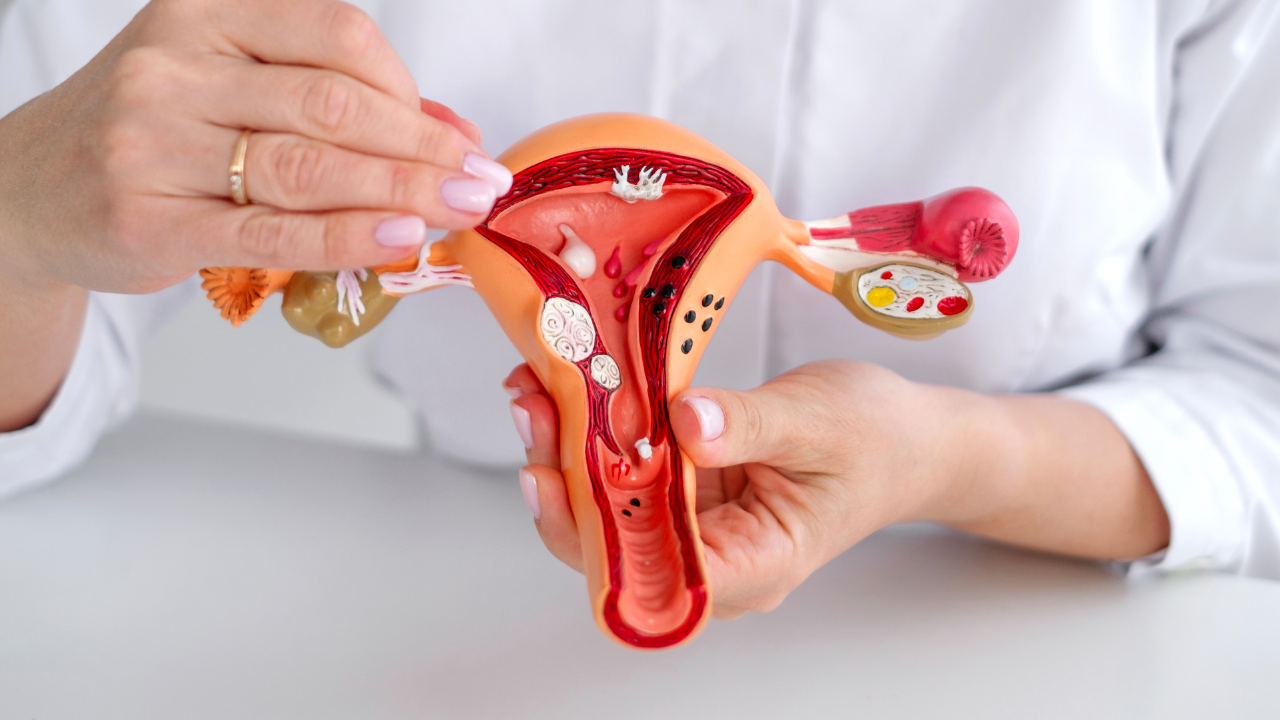
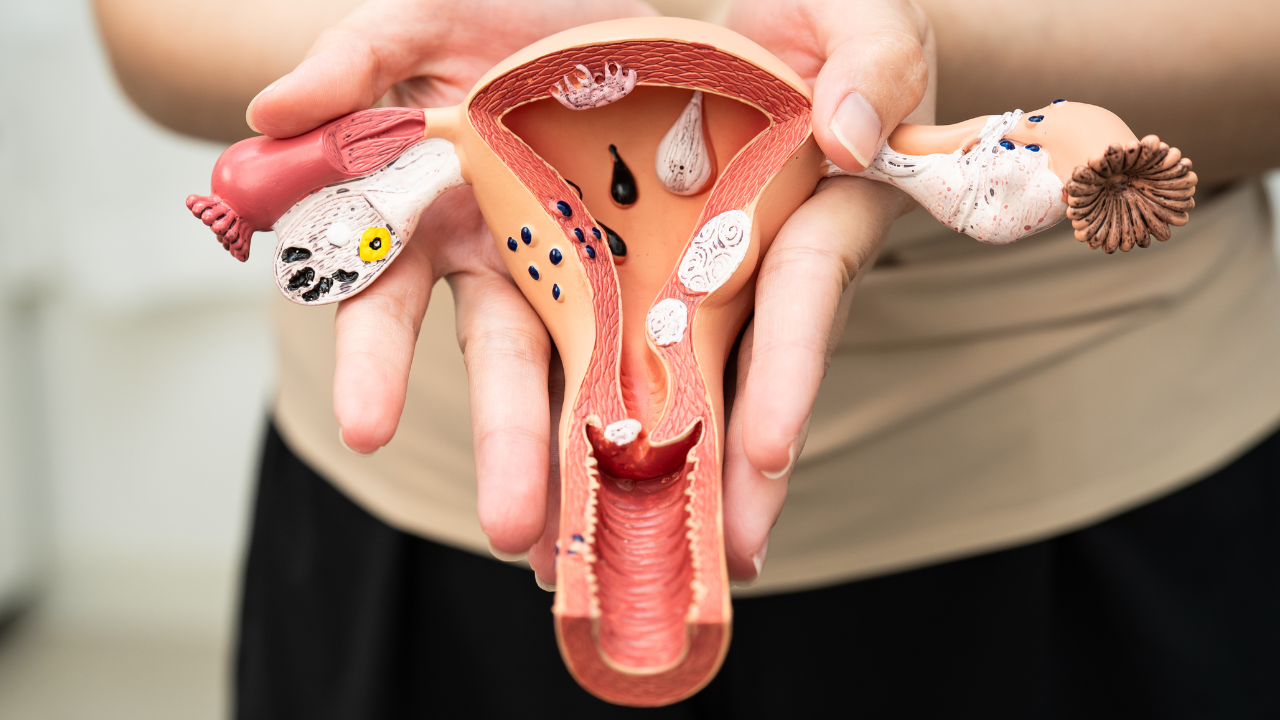
- Endometriosis diagnosis
While there are several causes of infertility, ovulation is a major factor. And, without ovulation there are no eggs to be fertilised, impeding on your ability to get pregnant.
Some signs of abnormal ovulation may include irregular or absent menstrual periods. Ovulation problems are often caused by PCOS, a hormone imbalance problem that can interfere with normal ovulation.
Other causes of infertility include:
- Blocked fallopian tubes due to pelvic inflammatory disease, endometriosis, or surgery for an ectopic pregnancy
- Physical problems with the uterus
- Uterine fibroids
When it comes to fertility, there are several factors beyond your control, but there are several things you can do to maximise your chances of conception:
- Maintain a healthy weight
- Stop or reduce smoking
- Avoid alcohol and recreational drugs
- Limit your daily consumption of caffeine
- Follow a sensible diet and exercise program
- Increase your daily intake of folic acid
- Visit your GP for an antenatal health check and review your prescription medications
- Avoid lubricants
- Manage stress
- Avoid exposure to toxins and use protective safety equipment in the workplace
“The journey for LGBTQ+ people, whether single or as a couple, is very often an assisted experience and a lot of thought, time, logistics and legalities is required to make it happen,” Dr Lieberman says.
“I would recommend that LGBTQ+ people engage a fertility provider or specialist that is welcoming and inclusive, offers services like egg and sperm donor banks and surrogacy support and has experience and expertise in supporting LGBTQ+ people realise their dreams of having a family.
When it comes to fertility health, Dr Lieberman says it’s important to bring men on the journey. “We have a lot of work to do to get men to realise they are equally likely to play a role in fertility health and infertility, particularly declining sperm count and quality.”
“Male fertility does decline with age, but not to the same extent as women and not until about 45 to 50. With men, it’s more about the increased risk of miscarriage and single-gene disorders like haemophilia and increased risk of schizophrenia and autism.”
“Men have an equally important role to play in achieving a healthy pregnancy. Their sperm needs to be just as healthy as women’s eggs to get the best chances of a pregnancy. This is just as true for sperm donors and surrogacy.”
Determining when you should seek professional advice for your fertility may seem daunting, that’s why accessing a patient-centred fertility clinic with expert specialists and world-class treatments is a sound approach.
As a general rule, if you are under 35 years of age and have been unable to conceive after 12 months of unprotected sexual intercourse, or after 6 months if over 35, you should seek advice from your GP or a fertility specialist.
“Unfortunately, there is still a lot of shame associated with not getting pregnant and it can be a lonely experience. I encourage women who are feeling like that to imagine that their best friend is going through it – and to consider what they would say to their best friend. Now is a good time to practice a bit of self-care and be kind to yourself.
“As a fertility specialist with many years working in family planning, I encourage people who are thinking about starting a family to get all of the information they need, whether they’re deciding to have children now or in the future, and to consider their options for any kind of treatment should they need it. Today there is a lot we can do to help,” Dr Lieberman said.